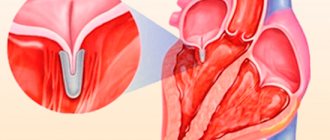
What is orthostatic hypotension?
Orthostatic hypotension is a pathological syndrome that is characterized by a sudden decrease in blood pressure due to a change in body position - rising from horizontal (lying or sitting) to vertical (standing).
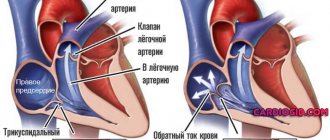
Directly related to decreased tone of the veins of the lower extremities. In this case, blood under the influence of gravity accumulates in the vessels of the lower extremities. Venous return to the heart, and then stroke volume, decreases, which leads to a decrease in pressure. Due to this phenomenon, cerebral blood flow is significantly reduced, which explains the symptoms of orthostatic hypotension:
- severe sudden weakness;
- flickering of spots, fogginess and darkening in the eyes;
- dizziness;
- syncope (fainting);
- noise, pulsation in the ears;
- nausea;
- rapid heartbeat (tachycardia).
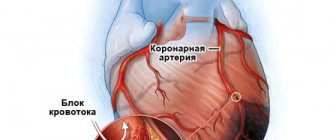
With prolonged fainting, due to oxygen starvation of the brain, convulsions and dysfunction of the pelvic organs may appear. It is not uncommon for a person to suffer a traumatic brain injury due to a fall. In this case, even after the return of consciousness, some symptoms do not disappear (headache, nausea). In patients with coronary heart disease, orthostatic collapse can provoke an attack of angina, which is also associated with impaired blood supply to the myocardium.
Externally, upon examination, you can detect such signs as pale skin, increased sweating. Most often, the condition occurs in the morning, after sleep, during prolonged standing in a stuffy room or in transport in the heat. If a person loses consciousness, they may experience short-term amnesia.
Depending on the severity and frequency of attacks, there are three degrees of orthostatic hypotension:
- I Art. (mild) – rare episodes with a complete absence of fainting;
- II Art. (moderate) – episodes are more frequent, fainting may occur;
- III Art. (severe) – almost every case ends in loss of consciousness.
If such a condition passes quickly and occurs only occasionally, this is considered a variant of the norm. This often happens during adolescence, when different organ systems develop unevenly.
However, if this syndrome occurs frequently, the manifestations do not disappear after 1-2 minutes, which may be a sign of pathological disorders in the body.
News
This is the name given to the development of fainting when loss of consciousness occurs after abruptly getting up from a place, remaining in a state of motionless standing for a long time, or performing heavy physical work.
What are the causes of orthostatic hypotension? Hypotension, or orthostatic shock, occurs due to dysregulation of blood pressure when it drops sharply and blood supply to the brain is reduced.
Orthostatic hypotension can develop in the following situations:
- decrease in the total volume of blood circulating in the body - hypovolemia,
- decreased cerebral vascular tone,
- exposure to certain medications and substances.
Hypovolemia can develop due to the loss of a large amount of blood due to injuries, bleeding, and in women - with heavy menstruation.
Blood plasma volume decreases with profuse sweating during fever and excessive physical exertion, especially in hot conditions.
A lot of fluid also leaves the body when there is excessive urination, which occurs during some diseases.
During vomiting and diarrhea, the body also loses fluid, which must be compensated.
All these factors lead to a decrease in the volume of circulating blood, as a result of which orthostatic collapse occurs.
The tone of cerebral vessels, especially their timely contraction and expansion, ensures the normal functioning of the body. Vascular tone is regulated by the nervous system. When this regulation is disrupted for one reason or another, orthostatic shock may develop.
Impairment of nerve fiber impulses occurs during a number of diseases, such as diabetes mellitus, vegetative-vascular dystonia, pulmonary artery thrombosis, atherosclerosis, anemia, adrenal tumors, as well as during prolonged bed rest.
Vascular tone can be altered by hormonal imbalances that occur during puberty, pregnancy and menopause.
Orthostatic shock can be a side effect of certain medications (antihypertensive drugs, fast-acting diuretics, nitrates, antiparkinsonian drugs, narcotics, etc.).
Risk factors:
- emotional stress,
- stress,
- depressive states,
- severe fatigue, including mental fatigue,
- physical, psychological,
- consumption of alcoholic beverages.։
What are the symptoms of orthostatic hypotension?
When suddenly rising from a lying position, after prolonged standing, as well as after excessive physical exertion, the following phenomena are observed:
- development of sudden severe general weakness,
- pale skin,
- dizziness,
- visual impairment (symptoms of tulle curtain, “midges”),
- possible nausea, vomiting,
- characterized by clouding of consciousness, fainting,
- possible limb spasms,
- At times there is involuntary urination.
How to diagnose orthostatic hypotension?
This condition is diagnosed by measuring blood pressure while standing (low) and lying down (normal), followed by comparison of the values.
Orthostatic hypotension is diagnosed if the difference is (in mmHg):
- systolic – 20 mm Hg. and higher,
- diastolic – 10 mm Hg. and higher.
In addition, pay attention to the presence of symptoms of cerebral circulatory failure - pallor, fainting, etc.
For diagnosis, a special test is used - an orthostatic test. It is carried out as follows - a person is placed on a rotating table and left to lie for 5 minutes, after which the table is sharply raised to a vertical position.
The following examinations are also carried out:
- clinical blood test (detection of anemia),
- biochemical blood test (assessment of the activity of internal organs),
- determination of hormones in the blood,
- examination of the heart condition, detection of autonomic disorders (Holter monitoring),
- neurological tests.
Treatment is prescribed depending on the mechanisms of development of the pathology.
Why is orthostatic hypotension dangerous?
Conditions of orthostatic hypotension cannot be ignored. They may be a manifestation of a serious pathology that requires treatment.
Constant oxygen starvation associated with insufficient blood supply to the brain is dangerous for memory deterioration and the development of neurological disorders. In older people, this condition threatens the development of stroke and dementia (dementia).
In addition, sudden fainting can cause injury due to a fall.
Some prevention techniques:
If symptoms develop, it is necessary to reconsider the regimen of medications taken due to the possible connection of symptoms with the side effects of these drugs.
You should not make sudden movements, you should avoid physical exertion, prolonged standing, and, if possible, emotional experiences.
If the patient has been on long-term bed rest, a gradual exit from such a regime is necessary. Before getting out of bed, you need to do a few simple exercises while lying down, then sitting.
In your diet, you need to somewhat limit meat dishes, especially fatty, hot spices. We must give up alcoholic drinks. You should drink enough water to avoid dehydration.
If episodes recur, you should consult a doctor!
What are the causes of the condition?
Under physiological conditions, the phenomenon occurs due to prolonged exposure to a supine position, fasting, and in high altitude conditions among climbers. Orthostatic collapse often develops during pregnancy, especially in the later stages. After childbirth, the normal state is restored.
As for the pathological causes of orthostatic hypotension, they can be as follows:
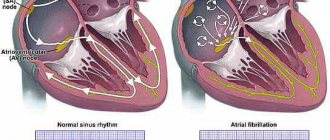
| Cardiopathology | Angina pectoris, chronic heart failure, valve defects and other structures, myocardiopathy, rhythm disturbances |
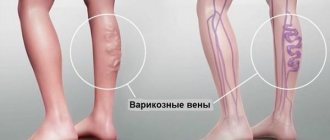
| Vascular diseases | Atherosclerosis, varicose veins of the lower extremities |
| Endocrine disorders | Diabetes mellitus, chronic adrenal insufficiency (Addison's disease), hypoglycemia due to insulin overdose |
| Neurological pathologies | Autonomic disorders, Parkinson's disease, amyloidosis, spinal cord injury, metabolic neuropathies, Shy-Drager syndrome |
| Adverse reactions from taking medications | Beta blockers, Viagra and its analogues, antidepressants, monoamine oxidase inhibitors |
| Postprandial hypotension | Blood pressure disturbances that occur after eating, especially in old age. |
| Dehydration | Both due to a decrease in water intake and as a result of an increase in consumption - due to vomiting, diarrhea, hyperhidrosis (increased sweating), blood loss; |
| Idiopathic hypotension | The exact cause cannot be determined |
How to treat?
If you witness an attack of orthostatic hypotension, you must provide first aid to the victim, which consists of the following:
- If a person has lost consciousness, sprinkle him with cold water or use ammonia (only very carefully, for example, moistening a napkin with a few drops of the solution, so as not to cause a burn to the nasal mucosa).
- When the patient returns to normal, give him warm tea with sugar.
- If consciousness does not return within one or two minutes, call an ambulance.
The following medications are used to treat manifestations of orthostatic hypotension:
- psychostimulants (caffeine preparations);
- alpha-adrenergic agonist (midodrine, etilephrine) – a hypertensive agent with a vasoconstrictor effect;
- mineralocorticoid (hydrocortisone) – helps increase circulating blood volume and constricts peripheral blood vessels.
- beta blockers (metoprolol, propranolol) – potentiate the effect of adrenal hormones;
- plant adaptogens (ginseng, eleutherococcus, lemongrass) – have a general tonic and strengthening effect on the body, increase blood pressure.
Specific therapy is also used for the specific disease that caused this syndrome.
Seizure prevention
An important part of the fight against this syndrome is prevention, which greatly reduces the frequency and severity of symptoms.
Doctors advise following the following recommendations:
- Avoid sudden changes in body position. When you wake up in the morning, lie down for a while and then slowly get up.
- If bed rest is indicated for you, take measures to combat physical inactivity. Do exercises right in bed, change your position periodically.
- If you have varicose veins, it is recommended to use compression bandages on the legs or special underwear;
- Maintain normal water balance - drink at least 1.5-2 liters of fluid per day. It is also necessary to consume enough salt.
- Walk more in the fresh air, engage in physical exercise (especially aimed at training the muscles of the legs and abdominals).
- Try not to overeat - this also provokes orthostatic collapse.
Are there any complications?
Pre-fainting states are far from harmless to the body. They can cause:
- injuries due to an unexpected fall of a person;
- stroke in older people;
- worsening of existing neurological pathology due to severe hypoxia of brain tissue;
- decreased memory, ability to learn, impaired intelligence;
- early senile dementia.
Manifestations of orthostatic hypotension should not be ignored. It can be the beginning of a serious brain pathology. Detection of the first symptoms requires careful diagnosis and monitoring of the implementation of preventive measures.
Does the presence of this condition affect the patient's overall prognosis?
It should be understood that orthostatic hypertension syndrome is not a separate disease, but usually develops against the background of one or another pathology and will always be an aggravating factor.
This condition can provoke the development of some dangerous complications. The most common are traumatic brain injuries due to falls. Another negative consequence may be encephalopathy, which occurs due to prolonged fainting, which can cause irreversible changes in the cerebral cortex, including dementia (dementia).
With proper treatment and implementation of preventive recommendations, the prognosis in most cases is favorable.
Indications for orthostatic test
The main objectives of an orthostatic test are to determine the relationship between observed symptoms and suspected diseases, clarify the diagnosis of latent hypertension, and help the doctor in selecting the dosage of certain medications. However, an orthostatic test is prescribed for diagnosis:
- coronary insufficiency;
- arterial hypertension;
- orthostatic hypotension;
- orthostatic tachycardia;
- dysfunction of the autonomic nervous system.
Also, samples of this type are necessary to monitor the patient’s condition during treatment with certain medications that cause circulatory disorders. Among such drugs are methyldopa, ganglion blockers, sympatholytics.
conclusions
Orthostatic hypotension, despite its apparent harmlessness, can lead to the development of dangerous complications, which, therefore, requires serious attention. If a rapid change in body position, in addition to slight dizziness or darkening of the eyes, is also accompanied by fainting, you should immediately consult a doctor for a full examination.
This condition may indicate the presence of diseases, such as pathologies of the cardiovascular system or endocrine disorders.
Diagnostics
Diagnosis of the condition of orthostatic hypotension is simple: the doctor measures blood pressure while lying and standing. Differences in performance are recorded. When rising, the pressure drops, and in a horizontal position it returns to normal.
In this case, the doctor may observe such signs as the patient turning pale and fainting. The condition is typical for rapidly growing adolescents. Often observed in boys at the commission at the military registration and enlistment office.
In specialized clinics, special placements on the table with fixation of the limbs and passive lifting to a vertical position are used.
In diagnosis, it is important to identify the cause of the condition. The criteria are typical signs:
- decrease in systolic pressure by at least 20 mm Hg;
- decrease in diastolic pressure by at least 10 mm Hg. Art.;
- the occurrence of an orthostatic collapsed state with dizziness and loss of consciousness.
A general examination allows us to identify indirect causes and is necessarily taken into account when making a diagnosis:
- a blood test can reveal anemia that the patient did not suspect;
- Among the biochemical tests, creatinine, sodium and potassium levels are important; they indicate renal filtration and the correct distribution of salts and water;
- the level of hormones such as cortisol, thyroid-stimulating hormone and others is determined in the blood, allowing one to study the function of the thyroid gland;
- with Holter monitoring, the ECG can be associated with food intake, sleep, and signs of autonomic disorders and a disrupted regulatory mechanism are revealed.
The patient is recommended to consult a neurologist to exclude the consequences of injuries and other diseases.
Special involvement of a neurologist is required if convulsions are observed when blood pressure drops