Features and advantages of vacutainers
The three-component system for venous blood collection consists of:
- sterile vacuum tube with preservative;
- double-sided automatic needle for intravenous injection;
- automatic needle holder.
The advantages of negative pressure systems are related to their design features:
- safety, sterility and guarantee of sample integrity;
- minimizing microclots and hemolysis;
- maintaining a constant time between collection and connection with the additive;
- exact ratio of sample and additive;
- minimizing the tourniquet effect.
Algorithm for taking blood using a vacuum system
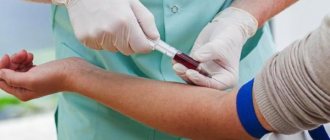
The method of collecting venous blood with vacuum tubes is similar to using a syringe, but provides greater safety, efficiency and convenience. The collection is carried out quickly, which is important to guarantee an accurate research result.
When collecting blood from a peripheral vein using a vacuum system, you will need:
- vacuum tubes;
- tourniquet;
- cotton wool (cotton swabs) or napkins;
- antiseptic (medicinal alcohol);
- bactericidal patch;
- sterile medical tray;
- medical clothing (gown, goggles, mask and gloves).
Before the procedure, it is necessary to fill out a patient referral, treat your hands with a special solution, and put on protective medical clothing.
Technique for collecting blood from a vein
- Prepare test tubes that correspond to the stated tests or laboratory tests required by the patient, a needle, a holder, alcohol wipes or a cotton swab, and a patch.
- Place a tourniquet on the patient's shirt or diaper 7-10 cm above the venipuncture site. Ask the patient to make a fist.
- Select a venipuncture site. The middle ulnar and saphenous veins are the most commonly used, but smaller and more plethoric veins of the dorsum of the wrist and hand can also be punctured.
- Take the needle and remove the cap from the rubber membrane side. Insert the needle into the holder and screw it in until it stops.
- Disinfect the venipuncture site with a gauze pad. You must wait until the antiseptic solution has completely dried.
- Remove the protective cap on the other side. Insert the holder-needle vacuum system into the vein in accordance with the algorithm for conventional blood collection using a syringe. Make sure that the needle is cut upward at an angle of 15º relative to the surface of the skin. Since the other end is covered with a membrane, blood does not flow through the needle. Using smooth and quick movements, the skin and vein wall are punctured. Deep immersion of the needle should be avoided.
- Insert the test tube as far as it will go into the holder. As a result, the needle pierces the membrane and the plug, and a channel is formed between the vacuum tube and the vein. The needle should not be moved when blood begins to flow. The process continues until the vacuum in the test tube is compensated.
- The tourniquet should be removed or loosened as soon as blood begins to flow into the vacutainer. Make sure the patient unclenches their fist.
- After the blood flow stops, the tube is removed from the holder. The membrane returns to its original position, the blood flow through the needle is blocked. If necessary, other tubes can be connected to the holder to collect the required volume of blood. Immediately after filling, the test tube must be carefully inverted to mix the sample with the filler: test tube without anticoagulants - 5-6 times; test tube with citrate - 3-4 times; test tube with heparin, EDTA and other additives - 8-10 times.
- After filling the last tube, disconnect it from the holder and remove the holder-needle system from the vein. To ensure safety, remove the needle from the holder and place it in a special container for disposal.
- A sterile napkin/cotton ball moistened with an antiseptic is applied to the puncture site, or a bactericidal patch is applied.
- The tubes are labeled and placed in a special container for transportation to the laboratory.
Manipulations at the preanalytical stage of laboratory research are the main source of errors and incorrect results. According to the literature, errors at the preanalytical stage are the cause of more than 60% of unreliable results. At the actual analytical stage of the study, according to the same data, no more than 20% of errors are introduced; Moreover, some of them are also due to previous disorders at the preanalytical stage (Fig. 1).
Figure 1. Number of errors identified at all stages of laboratory research, in %. M. Plebani and P. Carraro. 1348-1351 (1997).
The preanalytical stage begins much earlier than is usually described in textbooks. It must be remembered that any treatment process includes not only an assessment of the diagnostic value of the test, but also the need to prescribe monitoring, accompanying and additional procedures and studies. Therefore, the purpose of the study and the preparation of the patient for the collection of biomaterial should also be considered as components of the preanalytical stage.
Collection of biomaterial, transportation, storage and sample preparation are divided into non-laboratory and laboratory parts. The main task of these stages is to ensure the stability (safety) of the obtained biomaterials and minimize the influence of various factors that change their quality.
Proper preanalytical preparation is one of the main conditions for accurate laboratory diagnostics.
Currently, most clinics use a vacuum method of collecting venous blood. This method is as convenient as possible for both the patient and medical staff.
(Austria) is one of the leading manufacturers of vacuum systems for collecting biomaterial. Such systems ensure maximum safety for a medical worker when taking venous blood due to the fact that contact of blood with the environment is completely eliminated. However, even with good experience working with such systems, problems can sometimes arise.
Modern requirements for obtaining biomaterial are described in detail in the National Standards, however, in fulfilling these requirements, medical personnel often encounter a number of difficulties:
1. Blood does not flow into the test tube.
There may be several reasons for this, and each of them has its own solution:
2. During venipuncture, the blood flow suddenly stops quickly without filling the tube.
In this case, medical personnel should pay attention to the following possible causes and know how to solve the problem:
3. Hemolysis in vitro.
Hemolysis (damage to red blood cells during blood collection) is the process of damage to red blood cells in which hemoglobin is released from them into the environment. Blood or a suspension of red blood cells turns into a clear red liquid (“lacquered blood”). Hemolysis may render the sample unsuitable for analysis. The main causes and solutions to problems are as follows:
Let us dwell in more detail on the procedure for “direct” transfer of blood from a syringe into a vacuum tube, when the stopper is pierced with a syringe needle and the blood is forcefully squeezed out with a piston. This procedure has a number of disadvantages:
1. Sample transfer occurs under excess pressure, which leads to blood foaming, hemolysis and protein denaturation.
Denaturation of proteins:
— distorts the results associated with determining the activity and concentration of all proteins and enzymes, the activity of which directly depends on the spherical configuration of the protein molecule;
— leads to an increase in sample turbidity, which distorts the results of photometric techniques;
hemolysis is the main reason for the laboratory’s refusal to accept a sample for testing. Any hemolytic test is considered obviously incorrect.
2. Transferring a blood sample into a test tube with reagents necessitates precise dosing; when squeezing out blood with a piston, the test tube often overflows.
3. Handling an open needle carries the risk of injury to personnel from a contaminated needle.
Using a special holder to safely transfer blood from the syringe to the tube avoids these problems.
The syringe-to-tube blood transfer holder from the VACUETTE product line is designed for the correct transfer of blood samples from syringes. The design of the holder eliminates the risk of injury to medical personnel and facilitates blood transfer without additional manipulation. The holder complies with CLSI (Clinical and Laboratory Standards Institute) guidelines H3-A5. Follow these steps: draw a blood sample into a syringe using the procedure accepted in your medical institution (Fig. 2, a),
Figure 2. Holder for transferring blood from a syringe to a VACUETTE tube (a).
Explanation in the text. insert the test tube into the holder to transfer blood from the syringe to the test tube and press so that the holder needle pierces the stopper (Fig. 2, b),
Figure 2. Holder for transferring blood from a syringe to a VACUETTE tube (b).
Explanation in the text. as soon as the sample stops flowing into the test tube, carefully remove the test tube from the holder, continuing to hold it with your other hand (Fig. 2, c).
Figure 2. Holder for transferring blood from a syringe to a VACUETTE tube (c). Explanation in the text.
In addition, when studying a number of indicators, other errors are possible due to failure to comply with special requirements for the preanalytical process for this parameter.
1. Specific time of blood collection. In some cases, blood must be drawn at certain times: when taking certain medications, on an empty stomach and/or due to daily fluctuations in biological parameters (circadian rhythm). It is important that such samples are taken within a strictly specified period of time. The necessary instructions should be given to personnel performing venipuncture to ensure that these rules are strictly followed.
Examples of studies that require blood sampling at a certain period of time:
- studies of indicators that change during the day (for example, glucose, corticosteroids and other hormones, serum iron);
- monitoring of therapy (for example, prothrombin time, aPTT, concentration of salicylic acid, digoxin and other drugs).
In many of these situations, it is necessary to accurately record the dose of the drug and the time you last took it, as well as the time of the blood draw, on the referral form.
2. Features of blood collection for individual studies:
— determination of blood alcohol content. When taking a sample to determine blood alcohol content, disinfection of the venipuncture site should be carried out with an alcohol-free substance (for example, soap);
— samples for blood culture. When collecting, transporting and storing samples for blood culture, certain time and temperature conditions must be observed. In addition, there are differences in the volume of blood required for culture. Typically, one test requires taking 10-20 ml of blood from an adult and 1-2 ml of blood from a newborn;
- microelements. The VACUETTE product line includes special tubes for determining the concentration of trace elements.
3. Features of taking blood using catheters. There are a number of systems, the quality of which is of great importance when conducting laboratory diagnostics for patients in emergency clinics. This primarily concerns catheters and fistulas.
Possible mistakes
Indwelling catheters are usually placed in critically ill patients receiving massive fluid resuscitation. Taking blood samples from indwelling catheters may result in erroneous test results due to incomplete flushing of the entire length of the catheter. This results in contamination of the sample with drugs and/or dilution of the blood sample (Fig. 3).
Figure 3. Features of blood collection using catheters. The HOLDEX disposable holder is designed for use with VACUETTE butterfly needles, Luer needles or catheters.
Flushing catheters
Before collecting a sample, sufficient blood should be removed from the catheter to ensure that the sample is not diluted or contaminated. The volume of blood removed depends on the internal volume of the particular catheter. To study the hemostasis system, it is recommended to drain blood in an amount of at least 6 catheter volumes (5-7 ml), for other studies - at least 2 ml.
If a butterfly needle with a metal siliconized needle is installed in a patient in an emergency during emergency treatment for intravenous administration of drugs or for drawing blood, then it can be left in the vein for a period of 36 to 48 hours. Butterfly needles of the VACUETTE system (Austria) are intended for taking venous blood from children and patients with hard-to-reach veins for quick and painless venipuncture. The VACUETTE product line for venous blood collection includes both standard butterfly needles and SAFETY butterfly needles with a needle stick protection mechanism (Fig. 4).
Figure 4. Butterfly needles of the VACUETTE system (Austria) for the VACUETTE vacuum blood collection system.
Infusion therapy
If a patient is receiving intravenous fluids, blood should not be drawn from the same arm if possible. Blood collected proximal to the intravenous infusion site has been shown to be diluted with the injected solution. In addition, the solution may contain the analyte of interest. The results of the blood test in this case will be erroneous. It is necessary to find a place to draw blood on the other arm. Sometimes intravenous infusion can be given in both arms.
Satisfactory samples can be obtained by drawing blood distal to the intravenous infusion site. To do this, the following is recommended:
- turn off the IV at least 2 minutes before venipuncture;
— apply a tourniquet distal to the infusion site;
- choose a vein into which infusion is not carried out;
- perform venipuncture.
The referral form must indicate that the specimen was taken from the arm receiving the IV infusion.
If veins are not available, capillary blood collection is recommended.
Due to the possible occurrence of errors during research, taking blood from the intravenous infusion site should be avoided during the first 2 days after its discontinuation (Fig. 5).
Figure 5. Preparing the vein for infusion therapy.
In conclusion, it should be noted that in this article we have considered only some of the issues affecting the preanalytical stage. Problems associated with the preanalytical stage of laboratory research cannot be solved by one employee and require joint action by doctors, nurses and other laboratory personnel involved in the workflow of the medical institution. We hope that the errors discussed above that arise when working with vacuum tubes, and methods for solving them, as well as the peculiarities of taking venous blood, will allow readers to make a correct assessment and improve the quality of research.
Possible errors when using vacuum tubes
| Problem | Possible reasons | Solution |
| Blood does not flow into the tube after connecting to the holder | The needle did not enter the vein | In all of these cases, it is necessary to carefully adjust the position of the needle. There is no need to disconnect the tube from the holder if there is no need to remove the needle and under the skin. |
| The tip of the needle rests against the venous wall | ||
| The vein is pierced through | ||
| The blood in the test tube was received in less quantity than required for the analysis. | The venous vessel collapsed due to low pressure | It is necessary to disconnect the tube from the holder and wait a while until the vein is filled again |
| The system needs to be replaced and the procedure repeated | Air got into the test tube |
You can order high-quality laboratory consumables. When collecting blood using a vacuum system, follow the algorithm. This will ensure the safety of the procedure and the reliability of the research results.
Indications for the procedure
- Prescribed for the diagnosis of inflammatory diseases, infections, blood pathologies.
- Refers to a mandatory examination method during annual medical examinations.
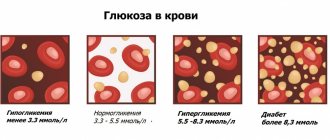
- Blood biochemistry determines the main biological indicators (glucose, proteins, electrolytes, enzymes, lipids) and indicates the pathology of the liver, heart, blood vessels, and the development of oncology.
- Hormonal background studies the level of hormones and the function of the endocrine, digestive system, and metabolism.
- The immunological status determines the state of cellular and humoral immunity, the development of allergic reactions.