Clinical use of fixed combinations of antihypertensive drugs
Currently, the issues of rational pharmacotherapy and the optimal choice of drugs for various diseases are of particular relevance, including cardiovascular diseases (CVD), which remain the leading cause of mortality throughout the world. The number of people with diseases of the cardiovascular system (CVD), according to modern foreign sources, exceeds 100 million. Every year, 16.7 million people worldwide die from CVD, and in almost 50% of cases the cause of death is coronary heart disease (CHD) and almost in 30% of cases - cerebral stroke (MI) [1]. Among CVDs, the most common is arterial hypertension (AH). It is this problem that practitioners most often have to deal with, and it is this that is a serious prognostic risk factor (RF) for the development of myocardial infarction (MI), MI, chronic heart failure (CHF), general and cardiovascular mortality [2].
In this regard, the issues of rational pharmacotherapy and optimal choice of drugs for CVD are of particular relevance. Based on evidence-based medicine, treatment algorithms for various CVDs are being actively developed. They are reflected in international and national clinical guidelines. The use of clinical recommendations in the practical work of a doctor undoubtedly helps to improve treatment results and prognosis for CVD [3, 4].
However, often prescribing optimal therapy is a difficult task, especially in the context of the expansion of the pharmaceutical market and the emergence of a large number of more and more new drugs (drugs), as well as due to the increasing prevalence of comorbid conditions, which in many ways complicate the implementation of drug therapy and require special close attention to monitoring the effectiveness and safety of drugs. As practice shows, the degree of compliance of the pharmacotherapy with accepted recommendations in real clinical practice remains quite low both in our country and abroad [5, 6].
In 2013, new recommendations of the European Society of Hypertension (ESH) and the European Society of Cardiology (ESC) for the treatment of hypertension were issued [7], as well as Russian recommendations “Diagnostics and treatment of arterial hypertension” [8 ], which are the basis for the selection of rational pharmacotherapy for hypertension by doctors of all specialties. The main goal of treatment of patients with hypertension is to minimize the risk of developing cardiovascular complications (CVD) and death from them. To achieve this goal you need:
- reducing blood pressure (BP) to the target level;
- correction of all modifiable risk factors (smoking, dyslipidemia, hyperglycemia, obesity);
- prevention, slowing the rate of progression and/or reducing target organ damage;
- treatment of associated and concomitant diseases (coronary artery disease, diabetes mellitus, etc.).
Choice of pharmacotherapy
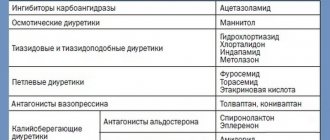
Currently, five classes of antihypertensive drugs with a proven effect on the degree of cardiovascular risk and no significant differences in the severity of the antihypertensive effect are recommended for the treatment of patients with hypertension:
- angiotensin-converting enzyme inhibitors (ACEIs);
- angiotensin II receptor blockers (ARBs);
- beta-blockers (BAB);
- calcium antagonists (CA);
- thiazide diuretics.
Each class has its own application features, advantages and limitations associated with the possibility of developing undesirable reactions.
The large arsenal of available drugs makes it extremely important and at the same time difficult to select specific drugs, and the differentiated choice of drugs remains a pressing problem for practicing physicians at the present time. This is especially true for patients who have additional risk factors and concomitant diseases, which, on the one hand, worsen the prognosis for hypertension, and on the other hand, limit the use of a number of antihypertensive drugs. Pharmacotherapeutic approaches to the treatment of patients with hypertension with concomitant risk factors and associated diseases require an integrated approach that makes it possible to influence not each disease separately, but the patient as a whole.
Of course, each patient requires serious thought and analysis of the characteristics of his clinical situation, and taking this into account, one or another class of drugs should be chosen. Recommendations summarizing the evidence base for all classes of antihypertensive drugs can be of great help to the practitioner at this stage. It is reasonable to consider certain drugs to be preferred for specific situations because they have been used in those situations in clinical trials or have demonstrated superior efficacy for specific types of target organ damage.
Adherence to treatment
When discussing the problem of rational pharmacotherapy of hypertension, one cannot help but dwell on its very important aspect - the low effectiveness of treatment of hypertension and failure to achieve target blood pressure (BP) values. This is explained by various factors, not the least of which is the low adherence of patients with hypertension to treatment. This is evidenced by the results of clinical and epidemiological studies conducted both abroad and in our country. Thus, according to various researchers, up to 50% of patients with hypertension independently stop treatment prescribed by a doctor [9, 10]. Low adherence to treatment is also evidenced by the results of the Russian multicenter study RELIF (Regular Treatment and Prevention), conducted in the Central and Northwestern Federal Districts, which showed that 58.2% of patients with hypertension take medications only when their blood pressure increases. Of these, 63.6% do not take drugs every day, 39.7% stop treatment after normalization of blood pressure, 32.9% skip doses due to forgetfulness, and only 3.3% do not skip medications [11].
Basic concepts of adherence to treatment
Adherence to treatment refers to the compliance of the patient's behavior with the doctor's recommendations, including taking medications, diet and/or lifestyle changes. Adherence to treatment involves concepts such as retention in therapy (persistence) and compliance.
Retention on therapy is determined by the length of time a patient receives drug therapy and is measured by the number of days a patient receives therapy or the percentage of patients who remain on treatment over a given period.
Compliance is an indicator of adherence to drug therapy (compliance with the dose, frequency and regimen). Compliance is assessed by the drug use index, which is the quotient of the number of days of taking the full dose of the drug (or its amount given to the patient) by the duration (in days) of the entire study (observation) period. Achieving 100% adherence seems to be the ideal goal, but this is difficult to achieve with any chronic disease. If the drug utilization index reaches 80% or more, compliance is considered acceptable.
In order to increase the information content of patient surveys regarding adherence to treatment, specialized questionnaires and scales for assessing adherence are being created. They, as a rule, include not only questions directly related to compliance with recommendations for taking medications and non-drug treatment methods, but also questions of a general psychological nature regarding the patient’s readiness to interact, responsibility, follow advice, etc. Some of these scales have now been validated and recommended for widespread use.
The simplest test for assessing compliance is the Morisky-Green test, consisting of four questions:
- Have you ever forgotten to take your medications?
- Are you sometimes inattentive to the hours of taking medications?
- Do you skip taking medications if you feel well?
- If you feel unwell after taking medication, do you skip the next dose?
Patients who score 4 points are considered compliant, and those who score less than 3 are considered non-compliant [12]. Using this simple and accessible method will help the practitioner pay attention to those patients who need additional attention in order to increase their compliance.
What are the ways to increase patients' adherence to treatment?
Today there is no single effective strategy for increasing compliance, however, when talking about the impact on treatment adherence, two main aspects should be kept in mind.
The first, concerning the patient’s actual adherence to the doctor’s recommendations, primarily depends on the motivation for treatment. In this aspect, the main efforts should be aimed at creating this motivation, which, first of all, requires establishing contact with the patient and training him. A number of authors and groups of experts, based on large analytical reviews of the literature, emphasize a fundamental change in the very approach to patient participation in the treatment process and more active involvement in medical decision-making. In their opinion, without the active participation and desire of the patient to be treated, it is difficult to achieve solutions to short- and medium-term, and even more so long-term problems.
It has also been proven that patients do not tend to follow doctor’s recommendations if they are not informed about their disease and its complications. Therefore, in this aspect, the main efforts should be aimed at creating a stable and high-quality doctor-patient relationship, at providing the patient with complete information about the disease and its complications in order to create motivation for strict and regular implementation of preventive measures and taking medications.
One of the ways to form a “doctor-patient” partnership is to educate patients, in particular in health schools for patients with hypertension, which essentially represent a medical preventive technology based on a combination of individual and group influence on patients and aimed at increasing the level of their knowledge, awareness and practical skills for the rational treatment of hypertension, increasing patient adherence to treatment and preventing complications of the disease, improving the prognosis and improving the quality of life.
The second aspect of adherence to therapy is the actual daily intake of drugs without significant deviations from the dose and regimen. This aspect can be significantly improved by simplifying the treatment regimen itself and introducing special techniques to help the patient not miss the next dose.
The need to use combination therapy for hypertension
The key point of modern antihypertensive therapy is combination therapy using rational combinations of drugs, which allows not only to achieve the target blood pressure level without reducing the quality of life of patients with hypertension, but also to reduce the risk of developing cardiovascular complications.
The results of a meta-analysis of large-scale clinical trials in recent years strongly suggest that to achieve target blood pressure and reduce cardiovascular risk (CVR), most patients need to be prescribed multiple antihypertensive drugs [13]. Combination therapy, in fact, is currently a priority in the treatment of patients with hypertension, which is reflected in the new European and Russian guidelines on hypertension [7, 8]. Combinations of two or more antihypertensive drugs are recommended to be prescribed to patients already at the stage of initial therapy, primarily to patients with high cardiovascular risk, i.e. patients with three or more risk factors, with subclinical target organ damage, as well as those with there are already associated clinical conditions.
Carrying out combination therapy for patients with hypertension seems justified and justified also due to the fact that, according to the mechanisms of development and formation, hypertension is a multifactorial disease, and the combination of drugs with different mechanisms of action, complementary to each other, makes it possible to optimally influence the various pathogenetic mechanisms of hypertension. A rational combination of drugs involves the use of drugs from different classes with different mechanisms of action in order to obtain an additional hypotensive effect and reduce the risk of adverse events. The combination of drugs with different mechanisms of action can also reduce changes in tissues, differently affecting the mechanisms of damage to target organs: the heart, blood vessels and kidneys.
Fixed drug combinations - a path to improving patient adherence
Increasing adherence to antihypertensive therapy is one of the most realistic ways to increase its effectiveness. Obviously, compliance with recommendations can only be achieved through cooperation between the doctor and the patient, which is largely achieved through detailed and at the same time accessible informing the latter about the purpose of treatment for hypertension.
The use of fixed combinations of antihypertensive drugs, which have become increasingly widespread in recent years, can also help improve adherence [14]. Clinical studies have shown that fixed combinations of small doses of antihypertensive drugs belonging to different classes are more effective than the use of the same drugs alone. Fixed combination drugs, for the creation of which improved dosage forms are used, are of great importance for rational pharmacotherapy. The advantages of fixed drug combinations are ease of prescription and dose titration, increased treatment efficiency and more frequent achievement of target blood pressure, convenience for the patient, improved patient adherence to treatment, as well as pharmacoeconomic advantages - improved cost/effectiveness ratio. The widespread use of fixed combinations of drugs already at the initial stage of treatment is a priority trend in the rational pharmacotherapy of hypertension today.
The advantages of fixed combinations are that they allow you to simultaneously influence different parts of the pathogenesis of hypertension. As a result, this approach to treatment makes it possible to achieve a more pronounced hypotensive effect compared to the use of monotherapy with drugs included in the combination drug, especially in cases where one of them sufficiently completely blocks the activation of counter-regulatory mechanisms caused by the action of the other component. This often eliminates the need to use high doses of individual drugs.
An important advantage of the use of fixed-dose combination antihypertensive drugs is improved patient compliance with the prescribed treatment regimen.
Most patients do not take medications regularly and often stop treatment for several days. Even in cases where patients take prescribed antihypertensive drugs, they do not always do so at the prescribed time. In a special study using electronic devices, it was shown that in 25% of patients, the time of taking the drug was 6 hours different from the one prescribed by the doctor. The greatest deviations from the prescribed therapy regimen are observed in cases where the drug dosage regimen is too complex or significant adverse drug reactions occur. Reducing the number of tablets taken daily to lower blood pressure is considered an important advantage of fixed-dose combinations. Moreover, if a combination drug has to be taken 2 times a day, the degree of compliance with the prescribed therapy regimen decreases, so preference is given to drugs that are effective when taken once a day.
To date, a large evidence base has been accumulated in the world to study the effectiveness, tolerability, benefits in terms of the effect on the state of target organs and cardiovascular indicators of various two-component combinations of antihypertensive drugs.
One of the relatively new combination drugs is the drug Concor AM, which is a fixed combination of a beta blocker (bisoprolol) and a dihydropyridine AK (amlodipine). Each of these drugs has been used in clinical practice for a long time and has a large evidence base.
Over the past 50 years, beta blockers have taken a strong position in the pharmacotherapy of the most common CVDs, and it is no longer possible to imagine modern cardiology without them. A large evidence base has made it possible to include this class of drugs in almost all modern recommendations - for the treatment of hypertension, coronary artery disease, and heart failure. They reduce the risk and frequency of CVD, have a positive effect on the clinical manifestations of the disease and improve the quality of life of patients with various CVD, as well as with concomitant pathology [7, 8].
The basis for the widespread use of beta blockers was the identification of the role of chronic hyperactivation of the sympathoadrenal system (SAS) in the development of endothelial dysfunction, left ventricular hypertrophy, malignant heart rhythm disorders and the progression of chronic heart failure. BBs are a very heterogeneous group of drugs in their pharmacological effects, within which there are significant differences in pharmacokinetics and pharmacodynamics regarding two main indicators - cardioselectivity and lipophilicity. A common property of all beta blockers is competitive antagonism of β1-adrenergic receptors. Along with blocking β1-adrenergic receptors, beta-blockers can also block β2-adrenergic receptors.
Experience in the clinical use of beta blockers in the treatment of hypertension indicates that they, especially β1-selective drugs, have fairly high antihypertensive efficacy and good tolerability when used long-term in average therapeutic doses in a wide variety of categories of patients [15–21].
Bisoprolol, which has high cardioselectivity, is widely used in clinical practice. If we take the ability to block β1 receptors in carvedilol as one, then for metoprolol this figure will be 6, for bisoprolol - 21 [22]. Also, being amphophilic, that is, soluble in both fats and water, bisoprolol has two elimination routes - renal excretion and hepatic metabolism. This ensures greater safety of use in patients with concomitant liver and kidney damage, elderly patients, as well as a low likelihood of drug interactions.
In terms of antihypertensive effect, bisoprolol is not only not inferior to other beta blockers, but is superior to them in a number of indicators. Thus, in the BISOMET study, it was shown that bisoprolol is comparable to metoprolol in terms of the degree of reduction in blood pressure at rest, but significantly exceeds it in its effect on the level of systolic blood pressure and heart rate during physical activity [23]. The effectiveness of bisoprolol in reducing cardiovascular risk in combination with the absence of a negative effect on carbohydrate metabolism has been proven in large randomized clinical studies, including such well-known ones as CIBIS-II (Cardiac Insufficiency Bisoprolol Study II) [24], TIBBS (Total Ischemic Burden Bisoprolol Study) [25], etc.
Amlodipine, which is part of Concor AM, is a third-generation AK, with a half-life of more than 35 hours, and has greater selectivity for coronary and cerebral vessels. The drug is practically devoid of inotropic effect and influence on the function of the sinus node, atrioventricular conduction, which determines its advantage over other AKs (the verapamil and diltiazem groups).
From the point of view of clinical pharmacology, the combination of a highly selective beta blocker and dihydropyridine AK is reasonable and justified. The effects of bisoprolol and amlodipine are complementary in reducing blood pressure, since they affect different parts of the pathogenesis, allowing for increased antihypertensive effectiveness: the vasoselective effect of amlodipine (reduction of total peripheral vascular resistance (TPVR)) and the cardioprotective effect of bisoprolol (reduction of cardiac output, reduction of heart rate) ), which in turn helps reduce the risk of developing pathological conditions in hypertension, such as angina pectoris, myocardial infarction, myocardial remodeling, and myocardial infarction [27].
In accordance with Russian recommendations for the treatment of hypertension, the primary indications for prescribing Concor AM are a combination of hypertension with coronary artery disease, atherosclerotic lesions of the carotid and coronary arteries, tachyarrhythmias, as well as isolated systolic hypertension, hypertension in elderly patients, and hypertension in pregnant women.
Clinical experience with the use of Concor AM indicates good antihypertensive efficacy of the drug with a high frequency of achieving target blood pressure values [26, 28, 29].
It is important to note that the studies conducted have demonstrated a good tolerability profile of the drug. Adverse events were mild and did not require discontinuation of the drug. Also, none of the ongoing clinical studies noted negative effects on carbohydrate and lipid metabolism [28, 29].
Important from a practical point of view is the fact that the drug is available in a wide range of doses of bisoprolol and amlodipine: 5 mg + 5 mg, 5 mg + 10 mg, 10 mg + 5 mg, 10 mg + 10 mg. This allows you to choose the optimal dosage regimen for each patient, taking into account individual hemodynamic characteristics.
Conclusion
Currently, the issues of rational pharmacotherapy and the optimal choice of drugs for various diseases are of particular relevance.
The quality of pharmacotherapy directly depends on the degree of patient adherence to treatment. Adherence is a key position linking the process and outcome of medical intervention. The use of fixed combinations of antihypertensive drugs in clinical practice simplifies the treatment regimen for patients with hypertension and helps improve adherence to treatment.
The drug Concor AM is a fixed combination of different doses of bisoprolol and amlodipine, has proven antihypertensive effectiveness in combination with a good safety profile. The components of the drug are complementary in relation to lowering blood pressure, since they affect different parts of the pathogenesis, allowing for increased antihypertensive effectiveness: the vasoselective effect of amlodipine (reduction of vascular resistance) and the cardioprotective effect of bisoprolol (reduction of cardiac output, decrease in heart rate), which in turn helps reduce the risk of developing pathological conditions in hypertension, such as angina pectoris, myocardial infarction, myocardial remodeling, cerebral stroke.
Literature
- https://who.int/gho/mortality_burden_disease/en/
- Shalnova S. A., Balanova Yu. A., Konstantinov V. V. et al. Arterial hypertension: prevalence, awareness, use of antihypertensive drugs and the effectiveness of treatment among the population of the Russian Federation // RKZh. 2006; 4:45–50.
- Wolf-Maier K., Cooper RS, Banegas JR, Giampaoli S., Hense HW, Joffres M. et al. Hypertension prevalence and blood pressure levels in 6 European countries, Canada and the United States // JAMA. 2003; 289:2363–2369.
- Redon J., Olsen MH, Cooper RS, Zurriaga O., Martinez-Beneito MA, Laurent S. et al. Stroke mortality trends from 1990 to 2006 in 39 countries from Europe and Central Asia: implications for control of high blood pressure // Eur Heart J. 2011; 32: 1424–1431.
- HYPERLINK “https://cardiotimes.com/2011/10/10/dramatic-underutilizationofproven-medications-for-cv-prevention/” Dramatic underutilization of provenmedications for CV prevention // /Lancet. 2011 (Published Online).
- Pogosova G.V., Koltunov I.E., Sokolova O.Yu. Secondary prevention of arterial hypertension and coronary heart disease in real clinical practice of the Russian Federation. M.: Vikas-print, 2009; 154 p.
- ESH/ESC Guidelines for the management of arterial hypertension // Journal of Hypertension. 2013, no. 31, pp. 1281–1357.
- Clinical guidelines “Diagnostics and treatment of arterial hypertension,” 2013. https://cardioweb.ru/klinicheskie-rekomendatsi.
- Conradi A. O. The importance of adherence to therapy in the treatment of cardiac diseases // Consilium medicum. Directory of a polyclinic doctor. 2007; 6.
- Pruijm MT, Maillard MP, Burnier M. Patient adherence and choice of antihypertensive therapy: focus on lercanidipine. Service of Nephrology and Hypertension, Department of Medicine, University Hospital, Lausanne, Switzerland // Vasc Heal Risk Management. 2008; 4(6):1159–1166.
- Pogosova G.V., Koltunov I.E., Melik-Oganjanyan G.Yu., Sokolova O.Yu. Adherence to the treatment of cardiovascular diseases: the problem of doctors and patients // Cardiovascular Therapy and Prevention, 2009; No. 4.
- Morisky DE, Green LW, Levine DM Concurrent and predictive validity of self-reported measure of medical adherence // Med Care. 1986; 24: 67–73.
- Wald DS et al. Combination Therapy Versus Monotherapy in Reducing Blood Pressure: Meta-analysis on 11,000 Participants from 42 Trials // Am. J. Med. 2009; V. 122. No. 3. P. 290.
- Morozova T. E., Yudina I. Yu. Modern strategy for improving adherence to treatment in patients with arterial hypertension: fixed combinations of drugs // Consillium medicum. 2010, vol. 22, no. 1, p. 22–28.
- Gurevich M. A. Modern approaches to the use of b-blockers // Economic Bulletin of Pharmacy. 2003. No. 3 (61). pp. 63–64.
- Metra M., Giubbini R., Nodari S. Differential effects of beta-blocers in patients with failure: a prospective, randomized, double-blind comparison of the longterm of metoprolol versus carvedilol // Circulation. 2000; 102(5):546–551.
- Wikstrand J., Hjalmarson A., Waagstein F. Dose of metoprolol CR/XL and clinical outcomes in patients with heart failure: analysis of the experience in metoprolol CR/XL randomized intervention trial in chronic heart failure // J Am Coll Cardiol. 2002; 40 (3): 491-49-84.
- Danhlof B. et al. Cardiovascular morbidity and mortality in the Losartan intervention for endpoint reduction in hypertension study (LIFE): a randomized trial against atenolol // Lancet. 2002; 359: 995-10-03.
- Efficacy of atenolol and captopril in reducing the risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 39. UK Prospective Diabetes Study Group // BMJ. 1998; 317(7160):713–720.
- Nuttall SL, Toescu V., Kendall MJ Beta-blockade after myocardial infarction // BMJ. 2003; 320(7234):581–588.
- Law MR, Morris JK, Wald NJ Use of blood pressure lowering drugs in the prevention of cardiovascular disease: meta-analysis of 147 randomized trials in the context of expectations from prospective epidemiological studies // BMJ. May 23, 2009; 338:b1665.
- Brixius K. et al. Nebivolol, bucindolol, metoprolol and carvedilol are devoid of intrinsic sympathomimetic activity in human myocardium // British Journal of Pharmacology. 2001; 133:1330–1338.
- Haasis R., Bethge H. Exercise blood pressure and heart rate reduction 24 and 3 hours after drug intake in hypertensive patients following 4 weeks of treatment with bisoprolol and metoprolol: a randomized multicentre double-blind study (BISOMET) // Eyr Heart Jour. 1987; 8; 103–113.
- CIBIS-II Investigators and Committees. The Cardiac Insufficiency Bisoprolol Study II (CIBIS-II): a randomized trial // Lancet. 1999; 353:9–13.
- Von Arnim T. Medical treatment to reduce total ischemic burden: Total Ischemic Burden Bisoprolol Study (TIBBS), a multicenter trial comparing bisoprolol and nifedipine // J Am Coll Cardiol. 1995; 25:231–238.
- Chesnikova A. I., Safronenko V. A., Kolomatskaya O. E. Evaluation of the effectiveness of a fixed combination of bisoprolol and amlodipne in the outpatient treatment of patients with arterial hypertension and coronary heart disease. Cardiology. 2014; 9:30–36.
- Stryuk R.I. Clinical rationale for the use of a fixed combination of bisoprolol with amlodipine for hypertension // Consilium medicum. 2013; 1:23–25.
- Rana R., Patil A. Efficacy and safety of bisoprolol plus amlodipine fixed dose combination in essential hypertension // Indian Pract. 2008; 61:225–234.
- Mehta S., Shah A. et fl. Efficacy and tolerability of a fixed dose combination of amlodipine and bisoprolol in essential hypertension // Indian Pract. 2005; 58: 751–759.
I. Yu. Yudina T. E. Morozova1, Doctor of Medical Sciences, Professor
GBOU VPO First Moscow State Medical University named after. I. M. Sechenova Ministry of Health of the Russian Federation, Moscow
1 Contact information
Hypotensive syndrome
Hypotensive syndrome is a whole complex of symptoms that reflects a persistent decrease in intracranial pressure in women. It occurs only in pregnant women aged 25 to 29 years. This syndrome significantly reduces the quality of life of the expectant mother and requires qualified medical care.
Make an appointment
Causes
The causes of this pathology are the following factors:
- severe dehydration after undergoing drug therapy;
- head injuries;
- leakage of cerebrospinal fluid due to a violation of the integrity of the skull bones or brain tissue;
- a decrease in blood pressure, leading to a decrease in intracranial pressure.
Every pregnant woman should be doubly attentive to her health, since she is also responsible for the life of the child. Any changes in health should be a reason to consult a doctor. Doctors at the Yusupov Hospital are ready to answer all their patients’ questions at any time, either in person or by phone.
Symptoms of hypotensive syndrome in pregnant women are:
- severe constricting sudden headaches;
- increased headaches when raising the head or in a sitting position;
- reduction in the intensity of headaches when lowering the head;
- prostration;
- feeling drowsy;
- irritability;
- attacks of nausea and vomiting.
Of course, many of the above symptoms occur in pregnant women and are a consequence of changes in the functioning of all organs and systems during the period of bearing a baby. They may have nothing to do with hypotensive syndrome.
But in any case, if the expectant mother’s health worsens, she must inform the doctor about it. Caution and attentiveness to your health will help you avoid the development of complications, identify hypotensive syndrome and undergo an effective course of therapy.
Diagnostics
If symptoms of the disease appear during pregnancy, it is necessary to undergo examinations by a gynecologist, neurologist and neurosurgeon. Doctors conduct examinations, analyze all the patient’s complaints and make a preliminary diagnosis. To confirm or refute it, the pregnant woman is prescribed a number of diagnostic measures, namely:
- general and biochemical blood test;
- general urine analysis;
- X-ray of the skull;
- spinal tap;
- MRI of the brain.
At the Yusupov Hospital, all diagnostic procedures are carried out using modern medical equipment, which allows you to obtain accurate data and promptly begin treatment.
Antihypertensive therapy: general rules
Both symptomatic hypertension and hypertension require correction with drugs that have a hypotensive effect. Antihypertensive therapy can be carried out with drugs that differ in their mechanism of action: antiadrenergic agents, vasodilators, calcium antagonists, angiotensin antagonists, and diuretics.
You can obtain information about the hypotensive effect of the drug and what medications to take for high blood pressure not only from your doctor, but also from your pharmacist.
Arterial hypertension is a chronic disease that requires constant drug support, daily monitoring and regular use of prescribed medications. Not only the state of health, but also the life of a person depends on compliance with these rules.
Despite the general availability of treatment rules for reducing blood pressure, many patients have to be reminded what a treatment regimen for hypertension should look like:
- Antihypertensive medications should be taken regularly, regardless of the patient’s well-being and blood pressure level. This allows you to increase the effectiveness of blood pressure control, as well as prevent cardiovascular complications and target organ damage;
- It is necessary to strictly adhere to the dosage and use the form of the drug prescribed by the attending physician. Independently changing the recommended dose or replacing the drug may distort the hypotensive effect;
- even if you are constantly taking antihypertensive drugs, it is necessary to systematically measure blood pressure, which will allow you to evaluate the effectiveness of therapy, timely identify certain changes and adjust treatment;
- in the case of an increase in blood pressure against the background of constant antihypertensive treatment - the development of an uncomplicated hypertensive crisis, an additional dose of a previously taken long-acting drug is not recommended. Blood pressure can be quickly reduced using short-acting antihypertensive drugs.